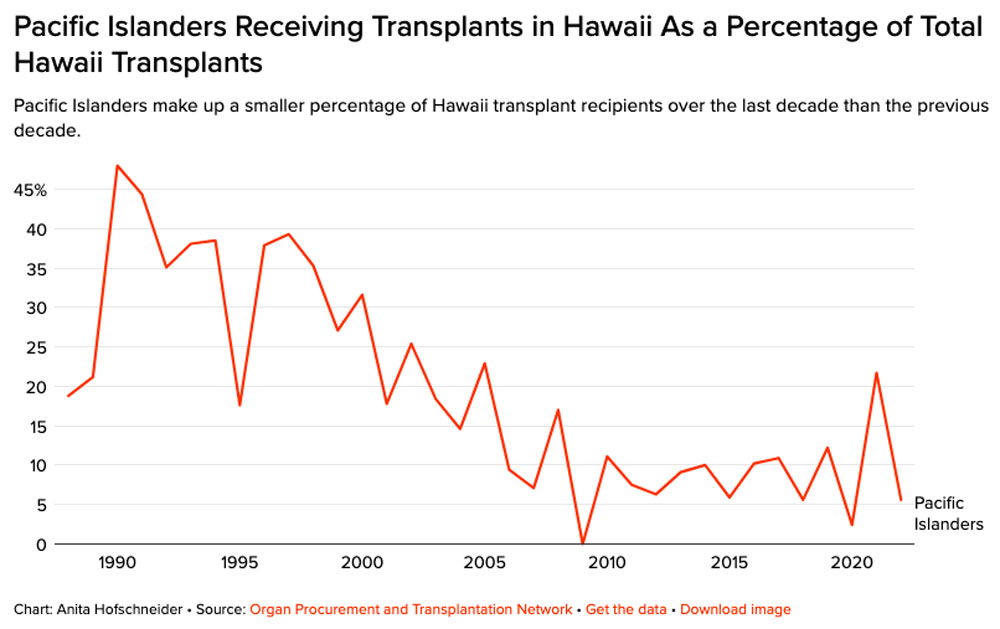
Getting kidney transplants is harder for Pacific Islanders
Editor’s Note: Reprinted from the “Journey to Care” series of the Honolulu Civil Beat. See the original post at https://www.civilbeat.org/2022/08/pacific-islanders-have-a-harder-time-getting-kidney-transplants-than-other-patients/
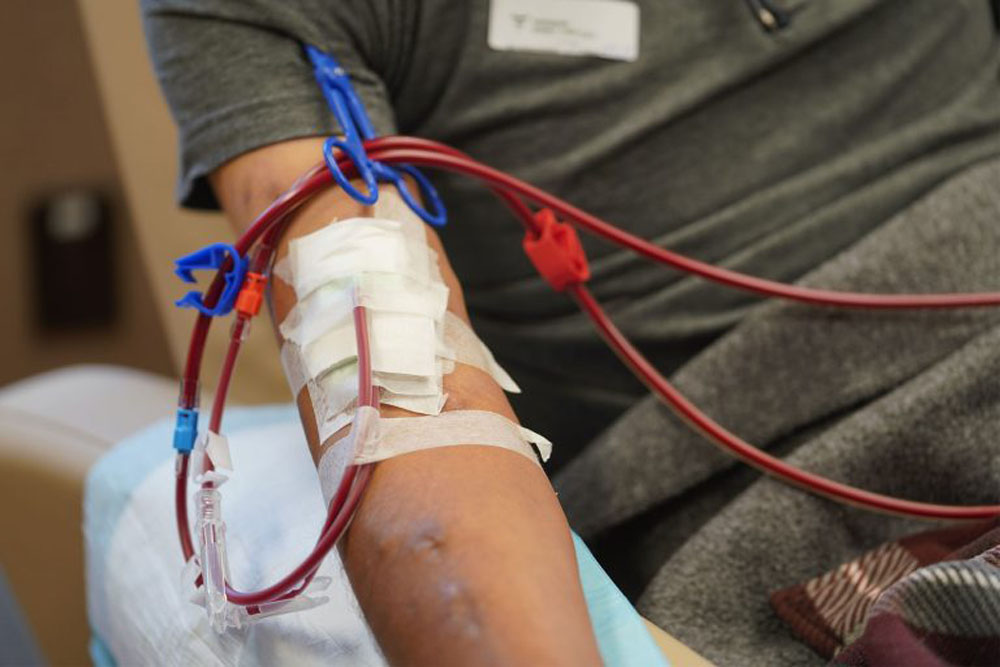
Just months into the COVID-19 pandemic, Ramona Beltran started a new weekly regimen: four to five hours of hemodialysis three times a week, a lengthy and exhausting blood-filtering process to do the work of her failing kidneys.
She waits for the Handi-Van in Laie to pick her up at 4:45am so that she can get to her appointment by 5:45am. She gets home between noon and 1pm, depending on traffic and how many other patients need to get dropped off along the way.
Her life revolves around medical appointments.
“I used to think I was superwoman,” she said. “I could come home and go back and do all the other things that I should do. But I can’t physically, my body just won’t move. And I notice that if I sit down and I want to do something, it takes me a while to get up and start moving.”
Beltran’s life has been irrevocably changed. But there’s something that could make it closer to normal—a kidney transplant. A new kidney would eliminate the need for long dialysis sessions, giving her back hours to spend with family or working.
But the 60-year-old Native Hawaiian woman hasn’t been able to get on the kidney transplant waiting list yet—she is still trying to meet the criteria.
A Civil Beat analysis of national data on end-stage renal failure and kidney transplants shows that people from Indigenous Pacific communities like Beltran who need kidney transplants are less likely to get them.
It’s particularly striking given that Pacific Islanders are disproportionately afflicted by kidney disease. Nationally, they were nearly six times more likely to need a kidney transplant in 2019 than would be expected by their share of the population, accounting for 1.19% of new end-stage kidney disease patients. Yet, they got only 0.27% of kidney transplants.
In other words, Pacific Islanders suffered from kidney failure at a rate four times higher than their rate of getting kidney transplants.
In comparison, white patients nationally made up more than half of new end-stage renal disease patients in 2019. But the number of kidney transplants for these patients was 20% higher than would be expected from their kidney failure rate.
Hawaii health care providers agree there are some legitimate reasons that many Pacific Islanders may get bypassed. Native Hawaiians and other Pacific Islanders are more likely to smoke and have other severe illnesses, conditions that can disqualify them from receiving transplants. Such criteria are in place to ensure transplants are successful.
But some providers say the strict criteria go too far and fail to account for cultural differences, such as requiring a main caregiver when Pacific Islander families often collectively care for their elders and sick loved ones. They note that body mass index limits don’t take into account muscle weight, and financial requirements may eliminate patients simply because they’re poor.
Critics say an overreliance on stringent criteria may effectively create structural barriers that amount to the same thing as discrimination, relegating many Pacific Islanders to suffering with little hope of relief.
“Even when it feels like we’ve done everything possible to prepare a patient for transplant evaluation and every team member from the pediatrician, nephrologist, mental health professionals to dialysis social workers believes a patient is ready and responsible for transplant, they are denied,” said Alicia Turlington, a physician at Kokua Kalihi Valley Comprehensive Family Services. “How can we not think of discrimination as a factor?”
Challenging criteria
Getting a new kidney isn’t easy for any patient. Patients must meet a long inventory of strict and subjective criteria to get on the waitlist. Then they often must wait years for a kidney that’s both functional and from a person with the right blood type.
In Hawaii, only The Queen’s Transplant Center in Honolulu does kidney transplants. Its medical director Alan Cheung says fewer people donate kidneys in Hawaii than in other places.



Cheung said the selection committee that evaluates waitlist applications for kidney transplants doesn’t consider race and ethnicity, and noted that patients from all backgrounds struggle with meeting the rigid requirements to qualify for a kidney.
Nationally, communities of color like Black and Latino Americans face well-documented disparities in kidney transplants. There’s a lot less research on Pacific Islanders, even though they have long been known to have disproportionately high rates of diabetes, hypertension, kidney disease and kidney failure.
Nephrologists and other health practitioners in Hawaii say despite the lack of data on Pacific Islanders and kidney transplants, they’ve noted the disparities.
Getting on the transplant waitlist is often the hardest part for patients, but even when it comes to getting the transplant itself, Pacific Islanders also appear to be at a slight disadvantage. In Hawaii, Pacific Islanders made up about 10.5% of people on the kidney transplant waitlist locally over the past 10 years, but just 9.4% of people getting them.
Queen’s took over the state’s only transplant center in 2011 from St. Francis Medical Center and in the decade since, the percentage of Pacific Islanders getting kidney transplants in Hawaii has fallen. The opposite is true for Asian patients, who over the last decade were more likely to get kidney transplants than Pacific Islander patients once they made the waitlist.
Cheung says that Queens hasn’t tightened its criteria since taking over from St. Francis and says the change might be due to better medical technology and online records that give providers more insight into patients’ overall health and make them more aware of factors that could disqualify them.
David Derauf, a physician and executive director at Kokua Kalihi Valley Comprehensive Family Services, who has been a physician in Hawaii for 30 years, estimates 60% of his Kalihi patients are Pacific Islanders.
Many struggle with diabetes, hypertension and kidney disease. But in the three decades he has worked at KKV, Derauf has never known a single patient with kidney failure who got a transplant.
“I am so eager to change that record,” he said. “Demonstrating that we can provide excellent equitable care for this condition will alleviate so much needless suffering in our community.”
Getting on the waitlist
The first step to getting a kidney transplant in Hawaii is getting on Queen’s waitlist. The hospital wouldn’t release a written copy of its criteria, but in interviews, Cheung detailed the transplant center’s policies.
The bottom line—those who want transplants must prove they’re model patients, consistently attending medical appointments and taking medication. They can be disqualified for having bipolar disorder and some other mental illnesses, as well as being homeless, conditions seen to make it less likely that they will follow post-transplant protocol.
They can’t do drugs or drink in excess or smoke.
That’s why Norvana “Cissy” Miranda hasn’t yet tried to get on the waitlist. The North Shore Oahu resident recently lost 70 pounds so she could qualify to start overnight at-home dialysis in April.
She knows kicking her smoking habit is the next step if she wants a new kidney. For now, the 66-year-old says, “One thing at a time.”
Apart from their failing kidneys, patients have to be in generally good health. Having a stroke or a heart attack can disqualify someone from getting on or staying on the list.
Both the BMI and the health requirements can be challenging to Native Hawaiians and other Pacific Islanders. Micronesians in particular are more likely to get sick at younger ages with serious illnesses such as cancer and heart disease than patients of Japanese ancestry, whites and even Native Hawaiians.
Native Hawaiians and other Pacific Islanders also are more likely to be homeless and have above-average poverty rates, making it harder to meet the financial requirements.
The reasoning behind the stringent transplant criteria, Cheung said, is that there are a limited number of kidneys and the transplant center wants to ensure the patients who receive them are successful. The federal government grades the center based on survival rates.
Robin Miyamoto, a physician and professor at the University of Hawaii John A. Burns School of Medicine, said Native Hawaiians and other Pacific Islander patients are more likely to get on dialysis in an emergency situation, which can be overwhelming and may not leave much time for adequate education about transplant options.
She and other health practitioners say a key factor is increasing culturally specific and linguistically appropriate education for patients with chronic kidney disease.
“In an ideal world, there would be a lot more funding for the education piece of things, but it’s really not rewarded by the current payment system,” she said.
Even though insurance may cover the transplant itself, post-transplant medications may cost patients thousands of dollars depending on what insurance plan they have. Patients must be vigilant about attending all appointments to make sure their bodies don’t reject their new organs.
Honolulu nephrologist Rick Hayashi said he understands why the requirements are so strict, given the brutal post-transplant recovery process. Still, he feels the requirements can make it difficult for people from immigrant or low-income backgrounds to get the necessary medical care.
The requirements are “somewhat of a barrier for access to care for socioeconomically disadvantaged patients, especially if they have no medical literacy or they don’t speak English, they only speak Chuukese or something,” Hayashi said.
Cultural and linguistic barriers
On its website, Queen’s offers a half-hour video describing the kidney transplant process but doesn’t provide the video or any other educational materials in languages other than English.
A 2018 state study found about 16% of Samoans, 18% of Tongans and 44% of Marshallese in Hawaii don’t speak English very well, compared with 12.5% of the state population overall.
Elisa Gordon, director of transplant surgery at Northwestern University Feinberg School of Medicine, said not translating materials into other languages is one way that communities of color are prevented from accessing kidney transplants.
She noted that some centers, such as the Hispanic Transplant Center at Northwestern, have embraced a culturally and linguistically sensitive approach to serving Spanish-speaking communities.
Cheung at Queen’s said that the center provides interpreters as needed for patients with low English proficiency.
Turlington from KKV feels that some of the transplant requirements don’t take into account cultural realities of Pacific Islander families. Turlington worked with a team of health care providers several years ago to submit an application for a kidney transplant for a Micronesian patient.
The team helped the family find stable housing in part so that they could meet the financial stability benchmarks. Turlington and her colleagues made sure the patient was consistently attending appointments before submitting the transplant application.
But the application was denied. Turlington says the main reason was because the patient hadn’t designated one individual to serve as caretaker. Instead, as was typical among Micronesian families, family members took turns taking time off work and driving the patient to and from appointments. Collectively, they ensured the patient was taken care of.
Turlington felt disappointed this was seen as a deficit, rather than a strength.
Cheung said the center encourages multiple caregivers but requires the patient to designate a lead. He said a single caregiver is important for continuity of care. When everybody is responsible, he said, nobody is.
David Naʻai, a nephrologist in Kailua, says a responsible Micronesian patient in her late 20s was denied a transplant solely because she couldn’t designate a main caregiver. The woman worked at Safeway and lived independently. Naʻai wishes people like her had more options, such as funding for a stay in a rehabilitation center.
Requiring a main caregiver is “very black and white,” Naʻai said, “especially in this environment that we live (in) here in Hawaii with different cultural practices and norms.”
His patient died a few years later in her early 30s.
Getting off the waitlist
Just making it to the waitlist is often the beginning of a much longer ordeal. Michael Kauhane was on the waitlist from 2015 to 2020. The Aiea resident developed diabetes and hypertension in 2005, which he blames on a combination of poor diet and exposure to Agent Orange while serving in Vietnam.
For five years, he did at-home dialysis every night from 9 p.m. until 7am, sleeping on his left side so that the tube could come out of his stomach and go into the machine by his bed. For years, he couldn’t fall into a deep sleep.
Some patients on the waitlist die or get transferred to different centers or get diagnosed with other illnesses that disqualify them from the list.
Thomas Aldan, a nephrologist in Honolulu, says some of his Pacific Islander patients who may be qualified for transplants decide against them for religious reasons, saying they believe God will provide for them. Or they’re put off by the potential costs, fearing an unknown price tag.
Elizabeth Kaleo, a Laie resident, is among those who wants to push forward with a transplant. She got on the list this year and prays every day that she’ll be blessed with a kidney.
But nationally, as in Hawaii, it appears that even Pacific Islanders like Kaleo who make the waitlist get kidneys at lower rates. Over the last decade, Pacific Islanders made up 4.7% of people on the kidney transplant waitlist nationally but just 4.2% of patients getting kidney transplants.
It’s a small disparity, but Darren Stewart, principal research scientist at the nonprofit United Network for Organ Sharing, said it could be partially driven by a lack of living donors who have blood types and tissue that match Pacific Islander patients.
Donors don’t need to be of the same race and ethnicity as recipients, but they do need to match blood types. Stewart said Asian Americans and Pacific Islanders are more likely to have blood type B, which can make it more difficult to find donors.
Also, kidney donors are often family members or friends, Stewart said. In communities beset with kidney disease, where people may expect to develop it themselves, fewer may be willing or able to donate the organ.
More research is needed, particularly about Pacific Islanders often left out of data collection and analysis, Stewart said.
The numbers at Queen’s may also reflect the availability of living donors in Hawaii. At Queen’s, only about 10% of kidneys come from living donors, Cheung said, compared to rates as high as 30% at other kidney centers. He said he isn’t sure why Hawaii’s donor rate is so low.
Difficult recovery
Miyamoto from the University of Hawaii thinks she may know the answer.
“When you have higher rates of chronic disease in the population, you’re just going to have less living donors that are available,” she said. Patients and potential donors also need paid sick leave to get enough time to recover, which many workers in Hawaii don’t have.
In 2020, Kauhane was admitted to Queen’s twice to prepare for a transplant. Each time there was a problem with the organ or another reason the surgery couldn’t happen.
Finally on Halloween, he got his transplant. Then came an intensive recovery process—his wife filled daily pill boxes with 97 medications and helped him get to appointments several times a week. Two years later, he’s down to about 20 medications but still has to be careful about what he eats to help his body accept the strange organ.
At age 72, Kauhane knows that death is not far off—but hopes now it won’t be from kidney disease. It has helped that Veterans Affairs has covered all the costs of his medication.
That’s not true for all patients, Miyamoto said. Medicare stopped covering the post-transplant medications for one of her Native Hawaiian patients so she ended up rationing her medications to stretch them longer. Her patient has since died.
Beltran, the Laie patient, looks forward to going down the same arduous road as Kauhane. Two years ago, a metal port in her chest from emergency dialysis prevented her from getting a mammogram required to make it to the waitlist.
“That was kind of sad, because I worked so hard trying to get all the appointments done,” she said.
She was told she would have to wait another year to try to get on the waitlist. She called last year to try to get on the list again but says she was told she couldn’t enroll in a necessary course because of the coronavirus pandemic.
In the meantime, she’s gotten used to going to dialysis, sitting in her recliner under the bright lights and bundling up in the cold air conditioning. She knows of others who have needed kidneys years before her and still haven’t had the transplants. Her cousin just died after six years of waiting for a transplant.
Still, she’s optimistic.
“I have my hopes up,” she said, “I might be able to go back to normal.”
This story was produced with support from the USC Annenberg Center for Health Journalism’s 2022 Impact Fund for Reporting on Health Equity and Health Systems, and Civil Beat supporter Dr. Mary Therese Perez Hattori.