Efforts to ‘flatten NMI’s curve’ holding strong
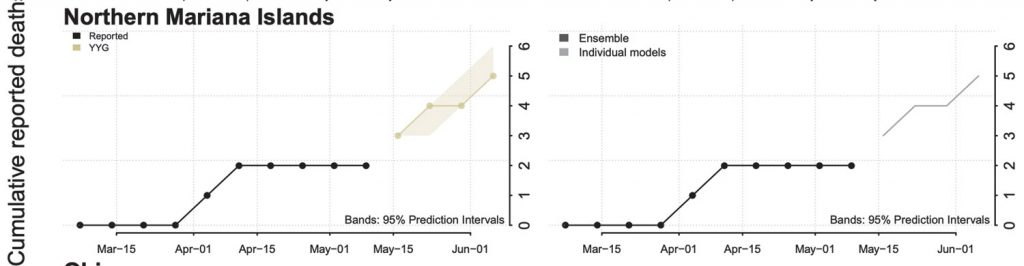
The CNMI has been putting in a comparatively solid effort in its fight against the COVID-19 pandemic, with just 21 cases since the outbreak in March, despite a grim projection of 3,000 positive cases by mid-June.
Citing prediction models, the Federal Emergency Management Agency had expected 3,676 positive cases in the CNMI by mid-June but that has not happened so far, according to Gov. Ralph DLG Torres, who cited the CNMI’s current seven active cases as an example of the CNMI’s early success is “flattening the curve.” The term refers to a public health strategy to slow the spread of COVID-19.
Torres credits the Commonwealth Healthcare Corp., its chief executive officer, Esther Muña; the Governor’s COVID-19 Task Force, and everyone else involved who have been working hard to control the spread of the coronavirus.
“Since Day 1, we’ve worked so hard in treating this pandemic as a high risk, even the fact that we had no cases. We were doing everything that even other states have not done,” said Torres during the governor’s media briefing on Monday.
Torres also pointed out that it’s not only just CHCC, the COVID-19 Task Force, and the front-liners that helped flatten the curve but also the community. “Everybody is in this fight,” said Torres.
According to Muña, there have been a lot of prevention and planning since January this year to help flatten the curve. She cited CHCC’s Public Health and Hospital Emergency Preparedness Program’s team for providing a list of actions that needed to take place. Muña stated that there were “key ingredients” to help flatten the curve which is: contact tracing, the ability to isolate individuals from the rest of the community, and the support of the CNMI government.
“Those are the things that were key to make sure that we have the capacity to manage what’s in front of us,” said Muña. “That really worked well with the COVID-19 Task Force, the medical team that we have, which is Dr. John Tudela, Dr. Beth Kohnen, Dr. Martin Rohringer, and basically coming together was really key to where we are now,” she said.
When asked to respond, people agreed to speak on the condition of anonymity.
“It’s still a little too early to say that the numbers will stay this way since the projection is in mid-June, but I personally think that if people continue to stay informed, alert, and cautious, then we won’t reach 3,000 cases by mid-June,” said Sally (not her real name)
“If a test was performed today and came out negative, that’s great but not really,” said Josh (not his real name). “Personally, I think that testing today does nothing to change the result of the virus being transmitted tomorrow to a person who tested negative today.”
Josh added that people can’t go around carelessly after they test negative. “Even if you tested negative, be mindful of the people around you and just keep up with staying home and not going out when you don’t need to,” he added.
The CNMI’s precautionary measures included stocking up on personal protective equipment, medical supplies, ventilators, UV lights for infection control, and the construction of an Alternative Care Site at the Kanoa Resort in Susupe and the Medical Care and Treatment Site at the upper parking lot of the Commonwealth Health Center.
According to Saipan Tribune’s archives, the modeling for the Marianas that was shared last April 14 suggested that COVID-19 positive cases are to exceed local capacity by late April, with peak hospitalization to occur in mid-June.
According to Delegate Gregorio Kilili C. Sablan (Ind-MP), the modeling comes from a briefing by Federal Emergency Management Agency Region IX administrator Bob Fenton that he presented to insular delegates on FEMA’s ongoing response to COVID-19 in the U.S. territories.
COVID-19 in Guam
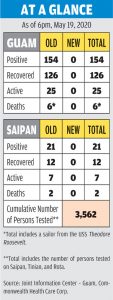
The Department of Public Health and Social Services tested 30 individuals for COVID-19 last May 18. All 30 tested negative.
To date, there have been 154 cases confirmed through COVID-19 testing in Guam, with five deaths and 126 released from isolation.
Cases are released from isolation under the following conditions: resolution of fever without the use of fever-reducing medications, improvement in respiratory symptoms and negative results from two consecutive respiratory specimens collected at least 24 hours apart.
Cases that test positive for COVID-19 through follow-up testing return to active isolation. All remaining cases are in isolation.